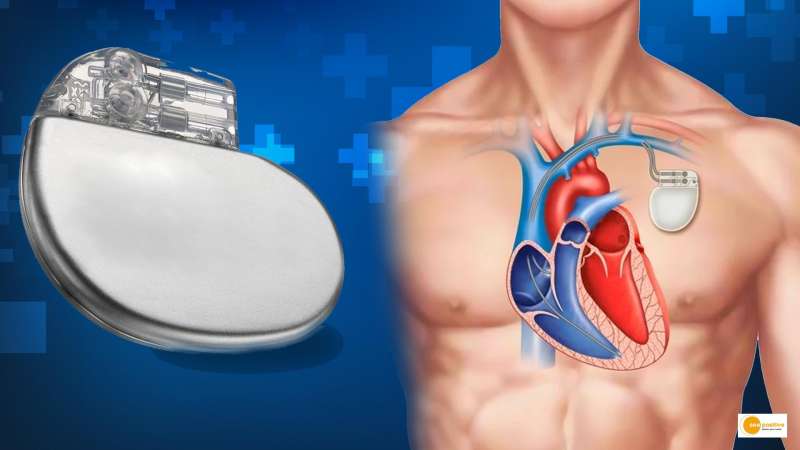
Several implantable devices have been developed as a result of rapid advances in information technology and medical sciences. The heart and related devices are discussed in this article, as they are used to provide cardiac resynchronization therapy, maintain rhythm, and prevent sudden cardiac death.
Personal healthcare shifted to home care, and finally to healthcare on the go
As a result, the use and popularity of fixed medical devices and systems is rapidly shifting to portable medical devices and systems, and eventually to wearable devices. The first-generation devices, such as the heart holter used to monitor and record cardiac activity, required user interaction to obtain and record data that was processed offline.
Several implantable devices have resulted from rapid progress in information technology and medical sciences. The heart and its associated devices are the focus of this article.
Pacemakers, implantable cardioverter defibrillators (ICDs), cardiac resynchronization therapy (CRT) devices, implantable loop recorders (ILRs), and implantable hemodynamic monitors are all examples of implantable electronic cardiac devices (IECDs) (IHMs). These devices are used to deliver cardiac resynchronization therapy, aid in rhythm maintenance, and prevent sudden cardiac death (see box).
A microprocessor is at the heart of each of the devices
When the microprocessor detects an event, it is programmed to collect data 24 hours a day and take the appropriate action. If the heart begins to beat too quickly, the device will deliver a therapy to restore the normal heart rhythm.
When a patient has the device implanted, it must be monitored on a regular basis.
The patient must visit the healthcare centre every three to six months for the device to be checked by the healthcare team. During the visits, the device’s data is downloaded to provide information about significant events such as device malfunction, arrhythmia, changes in hemodynamic status, or inadvertent changes in programmed parameters.
This allows for the evaluation of the therapy’s effects as part of a comprehensive cardiac evaluation and device optimization.
Remote monitoring technology’s evolution
In 1958, the first human pacemaker was implanted. The pacemaker did not last long, but the patient lived to be 88 years old, having had 26 pacemakers replaced in his lifetime. The development of demand pacemakers, which generated a regular electrical pulse without variation on their own when the heart was not beating regularly, marked the beginning of the modern era in 1969.
The process of remote monitoring
A sensing wand is placed over the device by the doctor during traditional follow-up visits to a health centre to download the data into a dedicated computer provided by the manufacturer. By analysing the data, the doctor can learn about what happened in the past, such as a high-energy shock or abnormal heart or device activity. Without the patient visiting the centre, remote monitoring makes information available wirelessly.
RF and electromagnetic interference
Implanted medical devices can use the Medical Implants Communication Services (MICS) frequency band, which ranges from 402 to 405MHz, to provide high-speed communication between patients’ IECDs and medical practitioners. The frequency is chosen based on the antenna efficiency and associated body losses.
In this regard, the 400MHz region offers optimization, with improved ability to transmit radio signals within the human body.